Understanding Septal Infarct: Causes, Symptoms, and Treatment
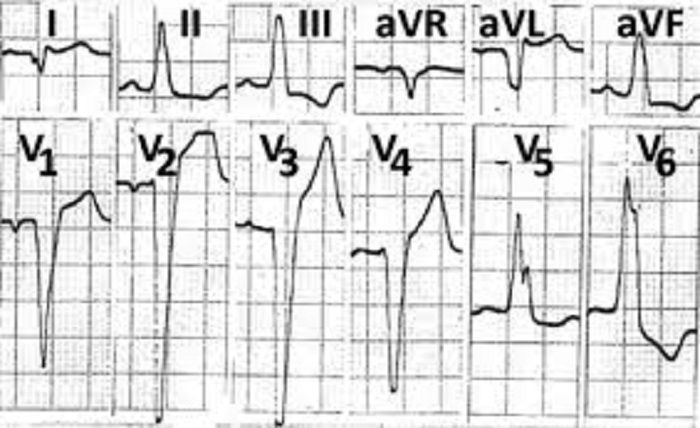
Septal infarct refers to a specific type of heart attack that affects the septum, the wall that divides the left and right ventricles of the heart. This condition can have serious implications on cardiac health and requires prompt medical attention. In this article, we will delve into the causes, symptoms, and treatment options for septal infarct, shedding light on this important cardiovascular condition.
What is Septal Infarct?
Septal infarct is a type of myocardial infarction, commonly known as a heart attack, which affects the septum. The septum plays a crucial role in maintaining the separation between the left and right ventricles of the heart. When blood flow to the septum is restricted or completely blocked due to a blood clot or plaque buildup in the coronary arteries, it can result in septal infarction.
Causes of Septal Infarct:
Septal infarct typically occurs due to coronary artery disease (CAD), where the coronary arteries become narrowed or blocked by atherosclerosis. The primary risk factors for CAD include smoking, high blood pressure, high cholesterol levels, diabetes, obesity, and a sedentary lifestyle. These factors contribute to the formation of plaque in the coronary arteries, leading to reduced blood flow and potentially causing a septal infarct.
Symptoms of Septal Infarct: The symptoms of septal infarct may vary depending on the severity of the condition. Common signs and symptoms include:
a) Chest pain: Individuals with septal infarct may experience severe, crushing chest pain that radiates to the left arm, jaw, or back. The pain can be persistent or intermittent.
b) Shortness of breath: Difficulty in breathing or shortness of breath, especially during physical exertion, may indicate septal infarct.
c) Fatigue and weakness: Feeling excessively tired or weak, even with minimal physical activity, is a possible symptom of septal infarct.
d) Dizziness and lightheadedness: Septal infarct can cause a drop in blood pressure, leading to dizziness and lightheadedness.
- Diagnosis of Septal Infarct: To diagnose septal infarct, healthcare professionals may perform various tests and examinations. These include:
Electrocardiogram (ECG): An ECG records the electrical activity of the heart and can identify abnormal patterns associated with septal infarct.
Echocardiogram: This test uses ultrasound waves to create images of the heart, helping to assess the structure and function of the heart’s chambers and detect any abnormalities in the septum.
Cardiac catheterization: This procedure involves the insertion of a catheter into the coronary arteries to evaluate blood flow and identify any blockages.
Treatment Options: The treatment for septal infarct focuses on restoring blood flow to the affected area of the heart and preventing further damage. Treatment options may include:
- a) Medications: Medications such as aspirin, beta-blockers, ACE inhibitors, and statins are commonly prescribed to manage symptoms, reduce blood clot formation, control blood pressure, and lower cholesterol levels.
- b) Percutaneous Coronary Intervention (PCI): PCI, also known as angioplasty, involves the insertion of a thin tube (catheter) with a balloon at its tip into the blocked coronary artery. The balloon is inflated to widen the artery and improve blood flow. In some cases, a stent may be placed to keep the artery open.
- c) Coronary Artery Bypass Grafting (CABG): CABG is a surgical procedure that involves grafting healthy blood vessels from other parts of the body to bypass the blocked or narrowed coronary arteries, allowing improved blood flow to the heart.
Conclusion:
Septal infarct is a serious condition that requires immediate medical attention. Understanding its causes, recognizing its symptoms, and seeking appropriate treatment can help minimize the risk of complications and improve outcomes. Maintaining a healthy lifestyle, managing risk factors, and following the prescribed treatment plan can contribute to the prevention and management of septal infarct. If you experience any symptoms associated with septal infarct, it is important to seek medical advice promptly to ensure timely intervention and the best possible care for your heart health.

